-

-

Location: Pittsburgh Marriot North or virtually via Zoom
For more information and to register click HERE
-

From L to R: Caitlin McNamara, MD, T32 Post-Doctoral Scholar
Erin Feeney, MD, PhD, Post-Doctoral Research Fellow, General Surgery Resident
Peter Nauka, MD, PACCM Fellow-PGY 5
Gitouf Elnema, MD, First Year IM Critical Care Fellow
-

Pioneers in Intensive Care Medicine
We are the nation’s first and foremost stand-alone department of critical care medicine.
-
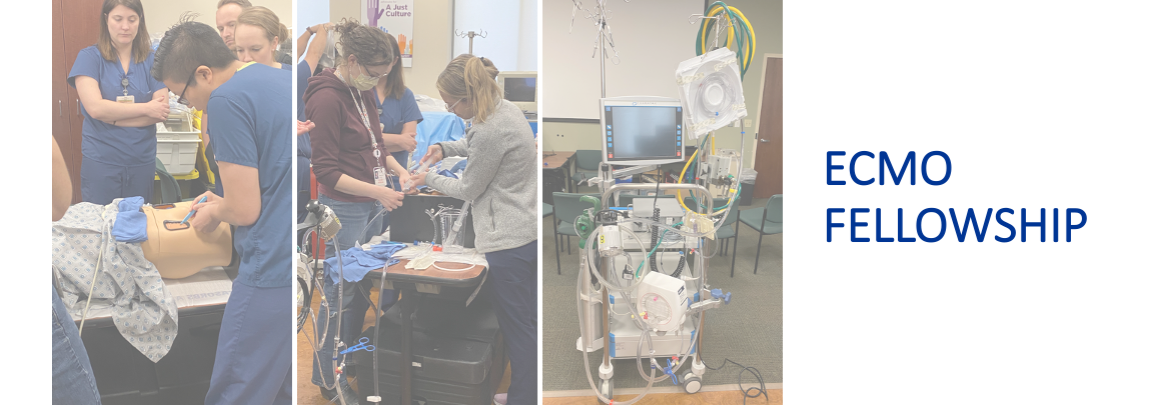
ECMO Fellowship
Now accepting applications for the 2024 term. Please see our ECMO Fellowship page for complete details.
A Message from the Chair
Welcome to the Department of Critical Care Medicine at the University of Pittsburgh and the UPMC Health System. We are a group of clinicians, teachers and scientists dedicated to improving the outcomes of patients who fall critically ill, and all those who care for them.
About Us

We provide state-of-the-art multidisciplinary care to critically ill adults and children

We train physicians and advanced practice providers to be leaders in critical care medicine.
We perform innovative, high-impact research across the translational spectrum.

Diversity, Equity & Inclusion
We value the richness of a diverse community of trainees, staff, physicians and investigators. Through collaboration, education, and active efforts to reinforce a culture of inclusion, our team members strive to:
- Respect the dignity of others
- Teach and learn from one another
- Promote inclusivity in the workplace
Our Beginnings
"We experienced the frustrations of trying to provide respirator care for unconscious patient care in various locations of the hospital without the help of trained inhalation therapists and specialty trained nurses. In 1958 therefore, we initiated and established an Intensive Care Unit adjacent to the post-anesthesia recovery room."
- Peter Safar, MD, cardiopulmonary resuscitation pioneer
